Why Does My Right Nut Hurt? If you’re experiencing discomfort in your right testicle, it’s natural to be concerned. At WHY.EDU.VN, we provide comprehensive information and expert insights to help you understand the potential causes and treatment options for testicular pain, including related conditions like groin pain and scrotal discomfort. Learn about potential causes and pain relief.
1. Unveiling the Mystery: Possible Reasons for Right Testicle Pain
Testicular pain, medically termed orchialgia, can stem from various underlying issues. Understanding the potential causes is the first step toward effective management. Here’s a breakdown of common reasons why your right testicle might hurt:
- Varicocele: Though more prevalent on the left side, a varicocele (enlarged veins in the scrotum) can occur on the right, causing a dull ache or throbbing sensation. Varicoceles affect approximately 10-20% of adolescent males, often developing during puberty.
- Epididymitis: Inflammation of the epididymis (the coiled tube at the back of the testicle that stores and carries sperm) can cause significant pain, often accompanied by swelling and redness. According to the CDC, epididymitis is most often caused by a bacterial infection, including sexually transmitted infections (STIs).
- Testicular Torsion: This is a medical emergency where the spermatic cord twists, cutting off blood supply to the testicle. It causes sudden, severe pain and requires immediate treatment to prevent testicular damage. The American Urological Association emphasizes that testicular torsion is most common in males between the ages of 12 and 18 but can occur at any age.
- Hydrocele: A hydrocele is a fluid-filled sac surrounding a testicle that causes swelling in the scrotum. Hydroceles are very common in newborn males and often disappear without treatment within the first year of life. Older boys and adult men can develop a hydrocele due to inflammation or injury within the scrotum.
- Testicular Cancer: Although less common, testicular cancer can sometimes manifest as pain or discomfort in the testicle. The American Cancer Society estimates that about 9,910 new cases of testicular cancer will be diagnosed in the United States in 2024.
- Inguinal Hernia: An inguinal hernia occurs when tissue, such as part of the intestine, protrudes through a weak spot in the abdominal muscles. This can cause pain and discomfort in the groin area, which may radiate to the testicle.
- Trauma: A direct blow or injury to the testicle can cause pain, swelling, and bruising.
- Kidney Stones: Pain from kidney stones can sometimes radiate to the groin and testicle area.
- Nerve Pain: Nerve damage or irritation in the groin area can also cause testicular pain.
It’s important to note that this is not an exhaustive list, and other less common conditions can also cause testicular pain.
2. Deciphering the Discomfort: Identifying Pain Characteristics
The nature of your pain can provide valuable clues about its underlying cause. Consider these factors when evaluating your discomfort:
- Onset: Did the pain start suddenly or gradually? Sudden onset pain is more likely to be associated with testicular torsion or trauma.
- Intensity: Is the pain mild, moderate, or severe? Severe pain warrants immediate medical attention.
- Location: Is the pain localized to the testicle itself, or does it radiate to the groin, abdomen, or back?
- Character: Is the pain a dull ache, a sharp stabbing sensation, or a throbbing pain?
- Aggravating Factors: What activities or positions worsen the pain? Pain that worsens with standing or exercise may suggest a varicocele.
- Relieving Factors: What helps to alleviate the pain? Rest, ice, or pain medication may provide temporary relief.
- Associated Symptoms: Are there any other symptoms present, such as swelling, redness, fever, nausea, or urinary problems?
Keeping a detailed record of your symptoms can help your doctor make an accurate diagnosis.
3. Varicocele: A Common Culprit Behind Left-Sided Pain
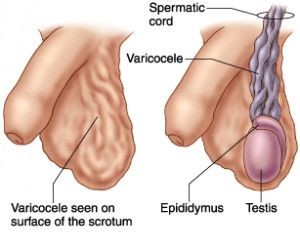 varicocele diagram
varicocele diagram
A varicocele is an enlargement of the veins within the scrotum, similar to varicose veins in the legs. While varicoceles are more common on the left side due to anatomical factors, they can occur on the right as well.
The exact cause of varicoceles is not fully understood, but they are thought to develop when valves inside the veins that regulate blood flow malfunction, leading to a backup of blood and subsequent vein enlargement.
3.1 Why the Left Side Predominates
The left spermatic vein drains into the left renal vein at a 90-degree angle, while the right spermatic vein drains directly into the inferior vena cava. This anatomical difference makes the left side more susceptible to increased pressure and backflow, contributing to varicocele formation.
3.2 Varicocele Symptoms and Diagnosis
-
Symptoms:
- A dull ache or throbbing pain in the testicle
- A feeling of heaviness or dragging in the scrotum
- Enlarged veins in the scrotum that may resemble a “bag of worms”
- Pain that worsens with standing or exercise and improves when lying down
- In some cases, infertility
-
Diagnosis:
- Physical examination: A doctor can often diagnose a varicocele by feeling the enlarged veins in the scrotum.
- Scrotal ultrasound: This imaging test can confirm the diagnosis and assess the size and extent of the varicocele.
3.3 Varicocele Treatment Options
- Observation: Small, asymptomatic varicoceles may not require treatment.
- Pain Management: Over-the-counter pain relievers, such as ibuprofen or acetaminophen, can help manage mild pain.
- Supportive Underwear: Wearing supportive underwear can help reduce pressure on the scrotum and alleviate discomfort.
- Varicocelectomy: This surgical procedure involves ligation (tying off) the affected veins to redirect blood flow.
- Varicocele Embolization: This minimally invasive procedure involves inserting a catheter into a vein in the groin or neck and using coils or other agents to block the affected veins.
Varicocele embolization, available at facilities that specialize in vascular procedures, offers a less invasive alternative to surgery, with a shorter recovery time.
4. Epididymitis: Inflammation and Infection
Epididymitis is inflammation of the epididymis, the coiled tube located at the back of the testicle that stores and carries sperm.
4.1 Causes of Epididymitis
- Bacterial Infection: This is the most common cause, often resulting from sexually transmitted infections (STIs) such as chlamydia or gonorrhea.
- Non-Infectious Causes: In some cases, epididymitis can be caused by non-infectious factors such as:
- Urine reflux into the epididymis
- Trauma
- Certain medications
4.2 Epididymitis Symptoms and Diagnosis
-
Symptoms:
- Gradual onset of pain in the testicle
- Swelling and redness of the scrotum
- Tenderness to the touch
- Fever
- Painful urination
- Discharge from the penis
-
Diagnosis:
- Physical examination: A doctor will examine the scrotum and testicles to assess for signs of inflammation and tenderness.
- Urine test: This test can help identify a bacterial infection.
- STI testing: If an STI is suspected, tests for chlamydia and gonorrhea will be performed.
- Scrotal ultrasound: This imaging test can help rule out other conditions, such as testicular torsion.
4.3 Epididymitis Treatment
- Antibiotics: If the epididymitis is caused by a bacterial infection, antibiotics will be prescribed. It’s crucial to complete the entire course of antibiotics, even if symptoms improve.
- Pain Management: Over-the-counter pain relievers, such as ibuprofen or acetaminophen, can help manage pain.
- Rest: Rest and elevation of the scrotum can help reduce inflammation.
- Ice Packs: Applying ice packs to the scrotum can also help reduce pain and swelling.
- Supportive Underwear: Wearing supportive underwear can help reduce pressure on the scrotum and alleviate discomfort.
5. Testicular Torsion: A Urological Emergency
Testicular torsion is a medical emergency that occurs when the spermatic cord twists, cutting off blood supply to the testicle. This can lead to irreversible testicular damage if not treated promptly.
5.1 Causes of Testicular Torsion
Testicular torsion typically occurs due to an anatomical abnormality that allows the testicle to rotate freely within the scrotum.
5.2 Testicular Torsion Symptoms and Diagnosis
-
Symptoms:
- Sudden, severe pain in the testicle
- Swelling of the scrotum
- Nausea and vomiting
- Abdominal pain
- The affected testicle may be higher than the other testicle
-
Diagnosis:
- Physical examination: A doctor will examine the scrotum and testicles to assess for signs of torsion.
- Scrotal ultrasound: This imaging test can help confirm the diagnosis and assess blood flow to the testicle.
- In some cases, surgery may be necessary to confirm the diagnosis.
5.3 Testicular Torsion Treatment
Testicular torsion requires immediate surgical intervention to untwist the spermatic cord and restore blood flow to the testicle. The surgery should be performed within 6-8 hours of the onset of symptoms to maximize the chances of saving the testicle.
6. Hydrocele: Fluid Accumulation
A hydrocele is a fluid-filled sac surrounding a testicle that causes swelling in the scrotum.
6.1 Causes of Hydrocele
- Congenital Hydrocele: This type of hydrocele is present at birth and occurs when the sac surrounding the testicle fails to close properly, allowing fluid to accumulate.
- Acquired Hydrocele: This type of hydrocele develops later in life due to:
- Inflammation or infection
- Trauma
- Testicular cancer (rare)
6.2 Hydrocele Symptoms and Diagnosis
-
Symptoms:
- Painless swelling of the scrotum
- A feeling of heaviness or fullness in the scrotum
-
Diagnosis:
- Physical examination: A doctor can often diagnose a hydrocele by feeling the fluid-filled sac in the scrotum.
- Transillumination: Shining a light through the scrotum can help confirm the diagnosis, as the fluid-filled sac will allow light to pass through.
- Scrotal ultrasound: This imaging test can help rule out other conditions, such as testicular cancer.
6.3 Hydrocele Treatment
- Observation: Small, asymptomatic hydroceles may not require treatment.
- Needle Aspiration: The fluid can be drained from the hydrocele using a needle. However, the hydrocele may recur after aspiration.
- Hydrocelectomy: This surgical procedure involves removing the hydrocele sac.
7. Testicular Cancer: A Less Common Concern
Testicular cancer is a relatively rare type of cancer that affects the testicles. While it can sometimes manifest as pain or discomfort in the testicle, it is often painless.
7.1 Risk Factors for Testicular Cancer
- Undescended Testicle (Cryptorchidism): This is the most significant risk factor.
- Family History: Having a family history of testicular cancer increases the risk.
- Age: Testicular cancer is most common in men between the ages of 15 and 35.
- Race: White men are more likely to develop testicular cancer than men of other races.
7.2 Testicular Cancer Symptoms and Diagnosis
-
Symptoms:
- A painless lump or swelling in the testicle
- A feeling of heaviness or dragging in the scrotum
- Pain or discomfort in the testicle (less common)
- Back pain
- Enlargement or tenderness of the breasts
-
Diagnosis:
- Physical examination: A doctor will examine the scrotum and testicles to assess for any abnormalities.
- Scrotal ultrasound: This imaging test can help confirm the presence of a tumor.
- Blood tests: Blood tests can help identify tumor markers that are associated with testicular cancer.
- Orchiectomy: This surgical procedure involves removing the testicle and is often necessary to confirm the diagnosis.
7.3 Testicular Cancer Treatment
Testicular cancer is highly treatable, especially when detected early. Treatment options include:
- Orchiectomy: Surgical removal of the affected testicle.
- Radiation Therapy: Using high-energy rays to kill cancer cells.
- Chemotherapy: Using drugs to kill cancer cells.
8. Groin-Related Causes of Testicular Pain
Pain in the testicle can sometimes be referred from other areas of the body, such as the groin.
8.1 Inguinal Hernia
An inguinal hernia occurs when tissue, such as part of the intestine, protrudes through a weak spot in the abdominal muscles in the groin area.
-
Symptoms:
- A bulge in the groin area
- Pain or discomfort in the groin, which may radiate to the testicle
- A feeling of heaviness or dragging in the groin
- Pain that worsens with straining or lifting
-
Treatment:
- Surgery is typically required to repair the hernia.
8.2 Kidney Stones
Pain from kidney stones can sometimes radiate to the groin and testicle area.
-
Symptoms:
- Severe pain in the back or side, which may radiate to the groin and testicle
- Blood in the urine
- Painful urination
- Nausea and vomiting
-
Treatment:
- Treatment depends on the size and location of the kidney stone and may include pain medication, increased fluid intake, or procedures to break up or remove the stone.
8.3 Nerve Pain
Nerve damage or irritation in the groin area can also cause testicular pain.
-
Causes:
- Surgery
- Trauma
- Infection
- Nerve compression
-
Treatment:
- Treatment may include pain medication, physical therapy, or nerve blocks.
9. Addressing Testicular Pain: When to Seek Medical Attention
It’s crucial to seek medical attention promptly if you experience any of the following:
- Sudden, severe pain in the testicle
- Swelling or redness of the scrotum
- A lump or mass in the testicle
- Fever
- Nausea or vomiting
- Pain that doesn’t improve with home treatment
- Any other concerning symptoms
A healthcare professional can accurately diagnose the cause of your testicular pain and recommend appropriate treatment.
10. Expert Advice and Personalized Solutions at WHY.EDU.VN
Navigating the complexities of testicular pain can be challenging. At WHY.EDU.VN, we strive to provide you with accurate, reliable, and easy-to-understand information to empower you to make informed decisions about your health.
10.1 Seeking Clarity and Guidance
If you’re struggling to find answers or need personalized advice, our team of experts is here to help. We understand the importance of addressing your concerns with sensitivity and expertise.
10.2 Addressing the Frustrations of Information Overload
We recognize the challenges of sifting through the overwhelming amount of information available online. That’s why we’ve created a platform where you can access credible and trustworthy resources.
10.3 Connecting with Experts and Seeking Reliable Answers
At WHY.EDU.VN, we’re committed to providing you with the knowledge and support you need to understand and manage your health concerns effectively.
FAQ: Addressing Common Concerns About Testicular Pain
Here are some frequently asked questions about testicular pain:
- Is testicular pain always a sign of a serious problem? Not always. While some causes of testicular pain require immediate medical attention, others are less serious and can be managed with conservative treatment.
- Can stress cause testicular pain? Stress can sometimes contribute to muscle tension and discomfort in the groin area, which may be perceived as testicular pain.
- Is it normal for one testicle to be larger than the other? It’s common for one testicle to be slightly larger or hang lower than the other. However, a significant difference in size or a sudden change in size should be evaluated by a doctor.
- Can exercise cause testicular pain? Exercise can sometimes aggravate certain conditions, such as varicoceles or inguinal hernias, leading to testicular pain.
- Is testicular pain always on the same side? Testicular pain can occur on either side, depending on the underlying cause.
- Can sitting for long periods cause testicular pain? Prolonged sitting can contribute to muscle tension and discomfort in the groin area, which may be perceived as testicular pain.
- How can I relieve testicular pain at home? Over-the-counter pain relievers, rest, ice packs, and supportive underwear can help alleviate mild testicular pain.
- When should I see a doctor for testicular pain? You should see a doctor if you experience sudden, severe pain, swelling, a lump, fever, or any other concerning symptoms.
- Can testicular pain affect fertility? Some causes of testicular pain, such as varicoceles, can affect fertility.
- Is testicular pain contagious? Testicular pain caused by a bacterial infection, such as epididymitis, can be contagious if the infection is sexually transmitted.
Conclusion
Experiencing pain in your right testicle can be unsettling, but understanding the potential causes is the first step toward finding relief. From varicoceles and epididymitis to the more serious concern of testicular torsion, it’s essential to seek prompt medical attention for an accurate diagnosis and appropriate treatment. Remember, early detection and intervention are crucial for preserving your health and well-being. For reliable information and expert guidance, turn to WHY.EDU.VN.
Do you have more questions or concerns about testicular pain? Don’t hesitate to reach out to the experts at WHY.EDU.VN. Our team is dedicated to providing you with the answers and support you need to navigate your health journey with confidence. Contact us at 101 Curiosity Lane, Answer Town, CA 90210, United States, or call us at Whatsapp: +1 (213) 555-0101. You can also visit our website at why.edu.vn to explore our extensive library of health resources and connect with our online community. We’re here to help you find the answers you’re looking for.