Why Does My Anus Hurt? This is a common question with a wide range of potential answers. At WHY.EDU.VN, we understand that discomfort in this area can be concerning and sometimes embarrassing to discuss, so we’re here to provide clear, reliable information about the potential causes of anal pain, burning, and itching, along with effective treatments and preventive measures. Explore comprehensive solutions and discover expert-backed advice for managing anorectal discomfort, finding lasting relief, and improving your overall anal health.
1. Understanding Anal Pain: Common Causes
Anal pain can stem from various sources, ranging from minor irritations to more serious underlying conditions. Identifying the root cause is the first step toward finding effective relief.
1.1. Hemorrhoids: Swollen Veins in the Rectum
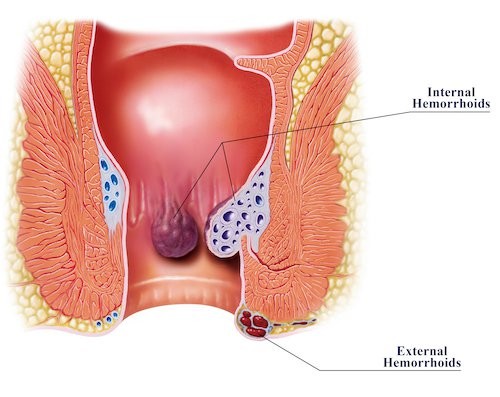
Hemorrhoids are one of the most frequent culprits behind anal discomfort. These swollen veins, located in the rectum and anus, can become irritated and painful, especially during bowel movements.
- Internal Hemorrhoids: Typically painless but may cause bleeding.
- External Hemorrhoids: Can cause throbbing pain, itching, and a noticeable lump near the anus.
1.2. Anal Fissures: Small Tears in the Anal Lining
Anal fissures are small cuts or tears in the lining of the anus. They often result from passing hard or large stools and can cause significant pain, especially during and after bowel movements.
- Symptoms: Sharp pain, burning sensation, and blood on toilet paper.
- Causes: Constipation, straining, and diarrhea.
1.3. Abscesses and Fistulas: Infections and Abnormal Connections
An anal abscess is a pus-filled pocket that forms near the anus or rectum. An anal fistula is an abnormal tunnel that connects the abscess to the skin around the anus.
- Abscess Symptoms: Pain, swelling, redness, and fever.
- Fistula Symptoms: Pain, drainage, and recurrent infections.
1.4. Pruritus Ani: Persistent Anal Itching
Pruritus ani, or chronic anal itching, can be caused by a variety of factors, including skin irritants, infections, and underlying medical conditions.
- Symptoms: Intense itching, burning, and soreness around the anus.
- Causes: Poor hygiene, excessive wiping, and certain skin conditions.
1.5. Proctitis: Inflammation of the Rectum
Proctitis is the inflammation of the lining of the rectum, which can lead to anal pain, bleeding, and discharge.
- Symptoms: Rectal pain, bleeding, diarrhea, and a feeling of urgency.
- Causes: Inflammatory bowel disease (IBD), infections, and radiation therapy.
1.6. Pelvic Floor Disorders: Muscle Spasms and Dysfunction
Pelvic floor disorders can cause a range of symptoms, including anal pain, due to muscle spasms and dysfunction in the pelvic region.
- Symptoms: Anal pain, pressure, and muscle spasms.
- Conditions: Levator ani syndrome, pelvic floor organ prolapse.
1.7. Anal Condyloma: Warts Caused by HPV
Anal condyloma, or anal warts, are caused by the human papillomavirus (HPV) and can lead to discomfort and itching in the anal area.
- Symptoms: Small, flesh-colored bumps around the anus, itching, and discomfort.
- Transmission: Sexually transmitted infection (STI).
1.8. Anal Cancer: A Rare but Serious Cause
While less common, anal cancer can also cause anal pain and bleeding. It’s essential to consult a healthcare professional for proper diagnosis and treatment.
- Symptoms: Anal pain, bleeding, changes in bowel habits, and a lump near the anus.
- Risk Factors: HPV infection, smoking, and a weakened immune system.
2. Diagnosing the Cause of Your Anal Pain
To accurately determine the cause of your anal pain, a thorough evaluation by a healthcare provider is crucial. This may involve a physical exam, a review of your medical history, and possibly some diagnostic tests.
2.1. Physical Examination: Visual Inspection and Palpation
A physical examination allows the healthcare provider to visually inspect the anal area for signs of hemorrhoids, fissures, or other abnormalities. Palpation, or feeling the area with a gloved finger, can help detect internal issues.
- External Examination: Visual inspection for hemorrhoids, fissures, and warts.
- Internal Examination: Palpation to detect internal hemorrhoids and masses.
2.2. Anoscopy and Sigmoidoscopy: Visualizing the Rectum and Anus
Anoscopy and sigmoidoscopy are procedures that use a small scope to visualize the inside of the anus and rectum, helping to identify the cause of pain, bleeding, or other symptoms.
- Anoscopy: Examination of the anal canal.
- Sigmoidoscopy: Examination of the lower part of the colon.
2.3. Colonoscopy: Comprehensive Examination of the Colon
A colonoscopy is a more comprehensive examination that allows the healthcare provider to view the entire colon, which can be necessary to rule out other potential causes of anal pain and bleeding.
- Purpose: To examine the entire colon for abnormalities.
- Indications: Persistent symptoms, family history of colon cancer.
2.4. Biopsy: Tissue Sampling for Further Analysis
In some cases, a biopsy may be necessary to collect a tissue sample for further analysis, especially if there are suspicious lesions or abnormalities.
- Purpose: To examine tissue samples for signs of cancer or other diseases.
- Indications: Suspicious lesions or abnormalities detected during examination.
3. Home Remedies and Self-Care for Anal Pain Relief
For mild to moderate anal pain, several home remedies and self-care measures can provide relief and promote healing.
3.1. Sitz Baths: Soothing Warm Water Soaks
Sitz baths involve sitting in warm water for 10-15 minutes several times a day. This can help soothe the anal area, reduce inflammation, and promote healing.
- How to: Fill a tub or sitz bath basin with warm water and sit in it for 10-15 minutes.
- Frequency: Several times a day, especially after bowel movements.
3.2. Fiber-Rich Diet: Promoting Regular Bowel Movements
Eating a diet rich in fiber can help prevent constipation and promote regular bowel movements, reducing strain on the anal area.
- Foods to Include: Fruits, vegetables, whole grains.
- Recommended Intake: 20-30 grams of fiber per day.
3.3. Hydration: Keeping Stools Soft
Drinking plenty of water helps keep stools soft and easier to pass, reducing the risk of anal fissures and hemorrhoids.
- Recommended Intake: At least 8 glasses of water per day.
- Benefits: Prevents constipation and reduces strain during bowel movements.
3.4. Over-the-Counter Creams and Ointments: Topical Relief
Various over-the-counter creams and ointments can provide temporary relief from anal pain, itching, and inflammation.
- Examples: Hemorrhoid creams, hydrocortisone creams.
- Benefits: Reduces inflammation and soothes irritated tissues.
3.5. Proper Hygiene: Gentle Cleansing After Bowel Movements
Proper hygiene is essential for preventing irritation and infection in the anal area. Gentle cleansing with mild soap and water after bowel movements is recommended.
- Technique: Use a soft cloth or moistened wipes.
- Avoid: Harsh soaps and excessive wiping.
4. Medical Treatments for Anal Pain
If home remedies are not sufficient to relieve your anal pain, medical treatments may be necessary. These can range from prescription medications to surgical procedures.
4.1. Prescription Medications: Stronger Relief for Pain and Inflammation
Prescription-strength creams and ointments can provide more potent relief from pain, itching, and inflammation.
- Examples: Topical corticosteroids, nitroglycerin ointment.
- Benefits: Reduces inflammation and promotes healing.
4.2. Stool Softeners and Laxatives: Easing Bowel Movements
Stool softeners and laxatives can help ease bowel movements and prevent constipation, reducing strain on the anal area.
- Types: Bulk-forming agents, osmotic laxatives, stimulant laxatives.
- Use: As directed by a healthcare provider.
4.3. Procedures for Hemorrhoids: Minimally Invasive Options
Various minimally invasive procedures can be used to treat hemorrhoids, including rubber band ligation, sclerotherapy, and infrared coagulation.
- Rubber Band Ligation: Placing a rubber band around the base of the hemorrhoid to cut off its blood supply.
- Sclerotherapy: Injecting a solution into the hemorrhoid to shrink it.
- Infrared Coagulation: Using infrared light to destroy the hemorrhoid tissue.
4.4. Surgery: Advanced Treatment Options
In severe cases, surgery may be necessary to treat anal fissures, fistulas, or other conditions causing anal pain.
- Lateral Internal Sphincterotomy (LIS): Cutting a small portion of the anal sphincter muscle to reduce pressure and promote healing of anal fissures.
- Fistulectomy: Surgically removing the fistula tract.
- Hemorrhoidectomy: Surgically removing hemorrhoids.
5. Preventive Measures for Maintaining Anal Health
Taking proactive steps to maintain anal health can help prevent anal pain and other related problems.
5.1. Maintaining a Healthy Weight: Reducing Pressure on the Rectum
Maintaining a healthy weight can reduce pressure on the rectum and anus, decreasing the risk of hemorrhoids and other conditions.
- Strategies: Balanced diet, regular exercise.
- Benefits: Reduces strain on the anorectal area.
5.2. Regular Exercise: Promoting Bowel Regularity
Regular physical activity can help promote bowel regularity and prevent constipation, reducing the risk of anal fissures and hemorrhoids.
- Recommended Activity: At least 30 minutes of moderate exercise most days of the week.
- Benefits: Stimulates bowel movements and reduces constipation.
5.3. Avoiding Straining During Bowel Movements: Gentle Elimination
Avoiding straining during bowel movements is crucial for preventing hemorrhoids and anal fissures. Take your time and allow for gentle elimination.
- Techniques: Relax and breathe deeply.
- Avoid: Forcing or straining.
5.4. Prompt Treatment of Diarrhea: Preventing Irritation
Prompt treatment of diarrhea can help prevent irritation and inflammation in the anal area.
- Strategies: Stay hydrated, eat bland foods, and consider over-the-counter anti-diarrheal medications.
- When to Seek Medical Attention: If diarrhea persists for more than a few days or is accompanied by severe symptoms.
5.5. Safe Sexual Practices: Reducing Risk of STIs
Practicing safe sex can help reduce the risk of sexually transmitted infections (STIs) that can cause anal pain and other symptoms.
- Recommendations: Use condoms, get vaccinated against HPV, and undergo regular STI screenings.
- Benefits: Prevents infections that can lead to anal discomfort.
6. Addressing Specific Conditions
Different conditions require specific approaches for effective management and relief.
6.1. Managing Hemorrhoids
- Increase Fiber Intake: Eat more fruits, vegetables, and whole grains.
- Stay Hydrated: Drink plenty of water.
- Use Topical Treatments: Apply over-the-counter hemorrhoid creams.
- Consider Sitz Baths: Soak in warm water to soothe the area.
6.2. Healing Anal Fissures
- Prevent Constipation: Use stool softeners and eat a high-fiber diet.
- Apply Topical Ointments: Use prescription-strength creams to relax the anal sphincter.
- Practice Good Hygiene: Clean the area gently after bowel movements.
6.3. Treating Abscesses and Fistulas
- Antibiotics: To treat infections.
- Incision and Drainage: To drain abscesses.
- Surgery: To repair fistulas.
- Warm Baths: To soothe discomfort.
6.4. Controlling Pruritus Ani
- Identify Irritants: Avoid harsh soaps, perfumes, and laundry detergents.
- Keep the Area Dry: Use zinc oxide ointments.
- Avoid Scratching: To prevent further irritation.
- Consult a Doctor: For prescription-strength medicated ointments.
6.5. Managing Proctitis
- Anti-inflammatory Medications: Oral or enema to soothe irritation.
- Sucralfate Enemas: To coat the lining of the rectum and reduce inflammation.
- Treat Underlying Conditions: Such as IBD or STIs.
6.6. Addressing Anal Condyloma
- Medical Procedures: To remove lesions.
- Regular Follow-Up: To monitor and treat anorectal cancer, especially in immunocompromised patients.
- HPV Vaccine: To prevent HPV infection.
6.7. Dealing with Pelvic Floor Disorders
- Physical Therapy: To strengthen pelvic floor muscles.
- Surgery: To support the pelvic floor muscles.
- Personalized Care Plans: To address specific needs.
7. The Role of Diet and Lifestyle
Your diet and lifestyle choices play a significant role in maintaining anal health and preventing pain.
7.1. Importance of Fiber
Fiber adds bulk to the stool, making it easier to pass and reducing strain on the anus.
| Food Source | Fiber Content (per serving) |
|---|---|
| Whole Grains | 3-5 grams |
| Fruits | 2-4 grams |
| Vegetables | 2-3 grams |
| Legumes | 6-8 grams |
| Nuts and Seeds | 2-4 grams |

7.2. Staying Hydrated
Water helps keep stools soft and prevents constipation.
- Recommended Intake: At least 8 glasses of water per day.
- Tips: Carry a water bottle and drink throughout the day.
7.3. Regular Exercise
Physical activity stimulates bowel movements and reduces constipation.
- Recommended Activity: At least 30 minutes of moderate exercise most days of the week.
- Examples: Walking, running, yoga.
7.4. Limiting Toilet Time
Spending too much time on the toilet can increase pressure on the anal area.
- Tips: Set a timer for five minutes.
- Avoid: Reading or using your phone while on the toilet.
8. Psychological Impact of Anal Pain
Living with chronic anal pain can take a toll on your mental and emotional well-being.
8.1. Anxiety and Stress
The constant discomfort and worry about bowel movements can lead to anxiety and stress.
- Strategies: Practice relaxation techniques, such as deep breathing and meditation.
8.2. Impact on Quality of Life
Anal pain can interfere with daily activities, work, and social interactions, affecting your overall quality of life.
- Solutions: Seek medical treatment and support to manage symptoms and improve well-being.
8.3. Seeking Support
It’s essential to seek support from healthcare providers, family, and friends to cope with the psychological impact of anal pain.
- Resources: Support groups, therapy, and online forums.
9. When to See a Doctor
While many causes of anal pain can be managed with home remedies, it’s important to know when to seek medical attention.
9.1. Persistent or Severe Pain
If your anal pain is persistent or severe, it’s essential to see a doctor to rule out more serious conditions.
9.2. Bleeding
Any rectal bleeding should be evaluated by a healthcare provider to determine the cause.
9.3. Changes in Bowel Habits
Changes in bowel habits, such as diarrhea or constipation, should be discussed with a doctor.
9.4. Fever
A fever accompanied by anal pain could indicate an infection and requires medical attention.
9.5. Suspicious Lumps or Growths
Any suspicious lumps or growths in the anal area should be evaluated by a healthcare provider.
10. FAQ About Anal Pain
1. What are the most common causes of anal pain?
Common causes include hemorrhoids, anal fissures, abscesses, and pruritus ani.
2. How can I relieve anal pain at home?
Home remedies include sitz baths, a high-fiber diet, and over-the-counter creams.
3. When should I see a doctor for anal pain?
See a doctor for persistent or severe pain, bleeding, or changes in bowel habits.
4. What is a sitz bath, and how does it help with anal pain?
A sitz bath involves sitting in warm water, which can soothe the anal area and reduce inflammation.
5. Can constipation cause anal pain?
Yes, constipation can lead to anal fissures and hemorrhoids, causing pain.
6. Is anal pain a sign of cancer?
While less common, anal pain can be a symptom of anal cancer, so it’s essential to get it checked by a doctor.
7. What is pruritus ani?
Pruritus ani is chronic anal itching that can be caused by various factors.
8. How can I prevent anal pain?
Preventive measures include maintaining a healthy weight, eating a high-fiber diet, and staying hydrated.
9. What are the treatment options for hemorrhoids?
Treatment options include home remedies, minimally invasive procedures, and surgery.
10. Can pelvic floor disorders cause anal pain?
Yes, pelvic floor disorders can cause anal pain due to muscle spasms and dysfunction.
Navigating anal pain can be uncomfortable, but understanding the potential causes and available treatments is the first step toward finding relief. At WHY.EDU.VN, we’re committed to providing you with accurate, reliable information to help you manage your health concerns.
Are you still struggling to find answers or relief from anal pain? Don’t hesitate to reach out to the experts at WHY.EDU.VN for personalized guidance and support. Visit our website at why.edu.vn or contact us at 101 Curiosity Lane, Answer Town, CA 90210, United States. You can also reach us via Whatsapp at +1 (213) 555-0101. Let us help you find the answers you need and the relief you deserve.