Why Do I Have Hemorrhoids? If you’re asking this question, you’re likely experiencing discomfort, and WHY.EDU.VN is here to provide answers. Hemorrhoids, also known as piles, are a common condition, but understanding the causes, symptoms, and effective treatments can bring significant relief. This comprehensive guide will explore the underlying reasons for hemorrhoid development, offering practical advice and solutions for managing this often-uncomfortable condition. Let’s explore various treatment options, including home remedies, lifestyle adjustments, and medical procedures to help alleviate symptoms and improve your overall well-being.
1. Understanding Hemorrhoids: A Comprehensive Overview
Hemorrhoids, also known as piles, are swollen veins in the anus and rectum that can cause pain, itching, and bleeding. While they can be uncomfortable and even distressing, understanding what they are and why they develop is the first step toward finding relief. They are a common ailment, affecting millions of people worldwide. Let’s delve deeper into the anatomy, types, and common misconceptions surrounding hemorrhoids.
1.1 What Are Hemorrhoids?
Hemorrhoids are essentially normal vascular structures within the anal canal that become problematic when they swell or become inflamed. Everyone has hemorrhoids, which consist of cushions of tissue filled with blood vessels located in the wall of the rectum and anus. These cushions help with stool control and support the tissues in the anal canal. Problems arise when these structures become enlarged, leading to the symptoms commonly associated with hemorrhoids.
1.2 Internal vs. External Hemorrhoids
There are two main types of hemorrhoids, classified by their location:
-
Internal Hemorrhoids: These occur inside the rectum and are usually painless, even when they bleed. Internal hemorrhoids are graded based on the degree to which they prolapse or protrude from the anus:
- Grade I: Do not prolapse; may cause slight bleeding.
- Grade II: Prolapse with straining but spontaneously reduce.
- Grade III: Prolapse with straining and require manual reduction.
- Grade IV: Chronically prolapsed and cannot be manually reduced.
-
External Hemorrhoids: These develop under the skin around the anus and are generally more painful, especially if a blood clot forms inside (thrombosed hemorrhoid).
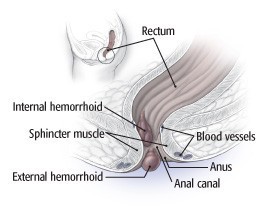 External Hemorrhoid Location
External Hemorrhoid Location
1.3 Common Symptoms
The symptoms of hemorrhoids can vary depending on the type and severity. Common symptoms include:
- Rectal Bleeding: Often painless, with bright red blood on toilet paper or in the toilet bowl.
- Itching: Irritation and itching around the anus.
- Pain: Discomfort or pain, especially during bowel movements or when sitting.
- Swelling: Noticeable swelling or a lump around the anus.
- Prolapse: Protrusion of hemorrhoids through the anal opening.
- Fecal Leakage: Difficulty cleaning after bowel movements, leading to soiling.
1.4 Debunking Common Myths
There are several misconceptions about hemorrhoids that can cause unnecessary worry:
- Myth: Hemorrhoids are always painful.
- Reality: Internal hemorrhoids are often painless, and pain usually occurs with external hemorrhoids or thrombosed hemorrhoids.
- Myth: Hemorrhoids lead to cancer.
- Reality: Hemorrhoids are not linked to cancer, but rectal bleeding should always be evaluated to rule out other potential causes.
- Myth: Only older people get hemorrhoids.
- Reality: While more common in older adults, hemorrhoids can affect people of all ages, including young adults and pregnant women.
- Myth: Hemorrhoid surgery is always necessary.
- Reality: Most cases can be managed with lifestyle changes and home remedies; surgery is reserved for severe cases or when other treatments fail.
2. Unraveling the Causes: Why Do I Have Hemorrhoids?
Understanding the underlying causes of hemorrhoids is crucial for effective prevention and management. Several factors can contribute to their development, ranging from lifestyle habits to physiological conditions.
2.1 Increased Pressure in the Lower Rectum
The primary cause of hemorrhoids is increased pressure in the lower rectum and anus. This pressure can lead to swelling and inflammation of the veins, resulting in hemorrhoid formation.
2.2 Common Contributing Factors
Several factors can increase pressure in the lower rectum and anus, including:
- Straining During Bowel Movements: Chronic constipation or diarrhea can lead to excessive straining, which puts pressure on the veins in the anal canal.
- Prolonged Sitting on the Toilet: Spending too much time on the toilet can cause the veins to swell and become inflamed.
- Chronic Constipation or Diarrhea: Irregular bowel habits can contribute to straining and irritation of the anal area.
- Obesity: Excess weight can increase pressure in the abdomen and rectum, leading to hemorrhoid development.
- Pregnancy: The growing uterus puts pressure on the pelvic veins, and hormonal changes can also contribute to hemorrhoids.
- Age: As you age, the tissues supporting the veins in the rectum and anus can weaken, making them more prone to swelling.
- Genetics: Some people may be genetically predisposed to developing hemorrhoids.
- Heavy Lifting: Repeatedly lifting heavy objects can increase pressure in the abdomen, contributing to hemorrhoids.
2.3 The Role of Diet
Diet plays a significant role in the development and management of hemorrhoids. A diet lacking in fiber can lead to constipation, which in turn causes straining during bowel movements.
- Low-Fiber Diet: Insufficient fiber intake leads to hard, difficult-to-pass stools, increasing the risk of hemorrhoids.
- Dehydration: Not drinking enough water can worsen constipation and exacerbate hemorrhoid symptoms.
2.4 Lifestyle Factors
Certain lifestyle habits can also contribute to hemorrhoid development:
- Sedentary Lifestyle: Lack of physical activity can lead to poor bowel function and increased risk of constipation.
- Poor Posture: Incorrect posture while sitting can increase pressure on the rectum and anus.
3. Identifying Risk Factors: Who is More Likely to Develop Hemorrhoids?
While hemorrhoids can affect anyone, certain groups are more susceptible. Understanding these risk factors can help in taking preventive measures.
3.1 Age and Hemorrhoids
The risk of developing hemorrhoids increases with age. As people get older, the tissues supporting the veins in the rectum and anus tend to weaken, making them more prone to swelling and prolapse.
3.2 Pregnancy and Hemorrhoids
Pregnancy is a significant risk factor for hemorrhoids. The growing uterus puts pressure on the pelvic veins, and hormonal changes can relax the veins, making them more susceptible to swelling. Additionally, straining during childbirth can exacerbate hemorrhoids.
3.3 Genetic Predisposition
Genetics can play a role in the development of hemorrhoids. If you have a family history of hemorrhoids, you may be more likely to develop them yourself.
3.4 Occupational Hazards
Certain occupations that involve prolonged sitting or heavy lifting can increase the risk of hemorrhoids. Truck drivers, office workers, and construction workers are examples of individuals who may be at higher risk.
3.5 Existing Medical Conditions
Certain medical conditions can also contribute to the development of hemorrhoids:
- Chronic Constipation: Conditions that cause chronic constipation, such as irritable bowel syndrome (IBS), can increase straining during bowel movements.
- Obesity: Excess weight puts additional pressure on the pelvic veins.
4. Recognizing the Symptoms: How Do I Know If I Have Hemorrhoids?
Identifying the symptoms of hemorrhoids is essential for timely diagnosis and treatment. Symptoms can vary depending on the type and severity of the hemorrhoids.
4.1 Common Signs and Symptoms
- Rectal Bleeding: This is one of the most common symptoms of internal hemorrhoids. You may notice bright red blood on the toilet paper, in the toilet bowl, or on your stool. Bleeding is usually painless.
- Anal Itching: Irritation around the anus can cause persistent itching. This symptom is more common with external hemorrhoids.
- Pain or Discomfort: Pain can range from mild discomfort to severe pain, especially during bowel movements or when sitting. External hemorrhoids are more likely to cause pain.
- Swelling or Lump: You may feel a lump or swelling around the anus. This is often associated with external hemorrhoids or prolapsed internal hemorrhoids.
- Prolapse: Internal hemorrhoids can protrude through the anal opening, especially during bowel movements. They may retract on their own or require manual repositioning.
- Fecal Leakage: Difficulty cleaning after bowel movements can lead to soiling or leakage of stool.
4.2 Differentiating Between Internal and External Hemorrhoid Symptoms
- Internal Hemorrhoids:
- Painless rectal bleeding
- Prolapse (protrusion of hemorrhoids through the anus)
- Discharge of mucus
- External Hemorrhoids:
- Pain and discomfort
- Itching
- Swelling or a hard lump around the anus
- Bleeding if a blood clot ruptures
4.3 When to See a Doctor
While many cases of hemorrhoids can be managed with home remedies, it’s important to seek medical advice in certain situations:
- Persistent Rectal Bleeding: Any persistent bleeding should be evaluated to rule out other potential causes, such as colorectal polyps or cancer.
- Severe Pain: Intense pain that doesn’t improve with home treatment may indicate a thrombosed hemorrhoid or another condition.
- Prolapse That Cannot Be Reduced: If an internal hemorrhoid prolapses and cannot be pushed back in, seek medical attention.
- Changes in Bowel Habits: Any significant changes in bowel habits, such as persistent constipation or diarrhea, should be evaluated.
- Anemia Symptoms: If you experience symptoms of anemia, such as fatigue, weakness, or shortness of breath, due to blood loss from hemorrhoids, see a doctor.
4.4 Diagnostic Procedures
A doctor can diagnose hemorrhoids through a physical examination and, if necessary, additional tests:
- Visual Inspection: The doctor will visually examine the anus to look for external hemorrhoids and signs of prolapse.
- Digital Rectal Exam (DRE): A gloved, lubricated finger is inserted into the rectum to feel for abnormalities.
- Anoscopy: A short, rigid tube with a light is inserted into the anus to visualize the anal canal.
- Sigmoidoscopy or Colonoscopy: If there’s evidence of rectal bleeding or microscopic blood in the stool, these procedures may be performed to rule out other causes of bleeding, such as colorectal polyps or cancer, especially in people over age 45.
5. Home Remedies: Simple Steps for Symptom Relief
Many cases of hemorrhoids can be effectively managed with simple home remedies. These treatments can help alleviate symptoms such as pain, itching, and swelling.
5.1 Dietary Changes
- Increase Fiber Intake: Fiber softens stools, making them easier to pass and reducing pressure on hemorrhoids. Good sources of fiber include fruits, vegetables, whole grains, and legumes. Aim for 25-30 grams of fiber per day.
- Stay Hydrated: Drink plenty of water to keep stools soft and prevent constipation. Aim for at least eight glasses of water per day.
5.2 Lifestyle Adjustments
- Avoid Straining: Try not to strain during bowel movements, as this increases pressure on the veins in the anal canal.
- Limit Time on the Toilet: Spending too much time on the toilet can cause the veins to swell. Limit your time to a few minutes per bowel movement.
- Maintain Regular Bowel Habits: Try to establish a regular bowel routine by going to the bathroom at the same time each day.
5.3 Topical Treatments
- Over-the-Counter Creams and Ointments: Hemorrhoid creams containing ingredients like hydrocortisone or lidocaine can provide temporary relief from pain and itching.
- Witch Hazel Wipes: Witch hazel has anti-inflammatory properties and can help soothe irritated skin.
- Sitz Baths: Sitting in a warm bath for 10-15 minutes several times a day can help relieve pain, itching, and spasms of the sphincter muscle.
5.4 Other Home Remedies
- Cold Compress: Applying a cold compress to the anal area for a few minutes can help reduce swelling and pain.
- Loose Clothing: Wearing loose, cotton clothing can help reduce irritation and promote air circulation.
- Avoid Irritants: Avoid using scented soaps, lotions, or wipes that can irritate the anal area.
5.5 Example Home Remedy Schedule
| Time | Activity | Benefit |
|---|---|---|
| Morning | High-fiber breakfast (e.g., oatmeal) | Softens stool for easier bowel movements |
| Mid-day | Drink 2 glasses of water | Keeps stool soft and prevents constipation |
| After Bowel Movement | Sitz bath for 10-15 minutes | Relieves pain, itching, and spasms |
| Evening | Apply over-the-counter hemorrhoid cream | Provides temporary relief from pain and itching |
| Before Bed | Drink 1 glass of water | Helps maintain hydration throughout the night |
6. Medical Treatments: When Home Remedies Aren’t Enough
When home remedies fail to provide adequate relief, medical treatments may be necessary. Several options are available, ranging from minimally invasive procedures to surgery.
6.1 Minimally Invasive Procedures
- Rubber Band Ligation: A small elastic band is placed around the base of the hemorrhoid to cut off its blood supply. The hemorrhoid shrinks and falls off within a week. This is one of the most commonly used treatments for internal hemorrhoids.
- Sclerotherapy: A chemical solution is injected into the hemorrhoid to shrink it. This procedure is less effective than rubber band ligation but may be an option for those who cannot tolerate banding.
- Infrared Coagulation: Infrared light is used to burn the hemorrhoid tissue, causing it to shrink. This procedure is generally painless and can be performed in a doctor’s office.
- Laser Coagulation: Similar to infrared coagulation, laser energy is used to destroy the hemorrhoid tissue.
- Electrocoagulation: An electrical current is used to coagulate the blood vessels in the hemorrhoid, causing it to shrink.
6.2 Surgical Options
- Hemorrhoidectomy: This is the traditional surgical removal of hemorrhoids. It is typically reserved for large, prolapsed hemorrhoids or those that have not responded to other treatments. Hemorrhoidectomy is effective but can be more painful and require a longer recovery period.
- Stapled Hemorrhoidopexy: A stapling device is used to reposition the hemorrhoids back into their normal position and reduce their blood supply. This procedure is less painful than traditional hemorrhoidectomy and has a shorter recovery time.
- Hemorrhoidal Artery Ligation (HAL): This procedure uses ultrasound to locate the arteries supplying blood to the hemorrhoids, which are then tied off to reduce blood flow and shrink the hemorrhoids.
6.3 Comparing Treatment Options
| Treatment | Type | Procedure | Pain Level | Recovery Time | Effectiveness |
|---|---|---|---|---|---|
| Rubber Band Ligation | Minimally Invasive | Elastic band placed around the base of the hemorrhoid | Mild | Few days | High |
| Sclerotherapy | Minimally Invasive | Chemical solution injected into the hemorrhoid | Mild | Few days | Moderate |
| Infrared Coagulation | Minimally Invasive | Infrared light used to burn the hemorrhoid tissue | Minimal | Few days | Moderate |
| Hemorrhoidectomy | Surgical | Surgical removal of hemorrhoids | High | 2-4 weeks | High |
| Stapled Hemorrhoidopexy | Surgical | Stapling device used to reposition hemorrhoids | Moderate | 1-2 weeks | High |
| Hemorrhoidal Artery Ligation | Surgical | Ultrasound used to locate and tie off arteries supplying blood to the hemorrhoids | Moderate | 1-2 weeks | High |
6.4 Choosing the Right Treatment
The best treatment for hemorrhoids depends on the type, severity, and individual factors. A doctor can help determine the most appropriate treatment plan based on a thorough evaluation.
7. Prevention Strategies: How to Avoid Hemorrhoids
Preventing hemorrhoids is often easier than treating them. By adopting healthy lifestyle habits and addressing risk factors, you can significantly reduce your chances of developing hemorrhoids.
7.1 Maintaining a High-Fiber Diet
- Include Fiber-Rich Foods: Eat plenty of fruits, vegetables, whole grains, and legumes. These foods add bulk to the stool, making it easier to pass and reducing straining.
- Consider Fiber Supplements: If you have difficulty getting enough fiber from your diet, consider taking a fiber supplement, such as psyllium husk or methylcellulose.
7.2 Staying Hydrated
- Drink Plenty of Water: Aim for at least eight glasses of water per day to keep stools soft and prevent constipation.
- Avoid Dehydrating Beverages: Limit your intake of caffeine and alcohol, which can dehydrate the body and contribute to constipation.
7.3 Practicing Good Bowel Habits
- Avoid Straining: Try not to strain during bowel movements. If you are constipated, try increasing your fiber and fluid intake.
- Limit Time on the Toilet: Spending too much time on the toilet can cause the veins to swell. Limit your time to a few minutes per bowel movement.
- Respond to the Urge: Don’t ignore the urge to have a bowel movement. Delaying can lead to harder stools and increased straining.
7.4 Lifestyle Modifications
- Regular Exercise: Physical activity helps stimulate bowel function and prevent constipation. Aim for at least 30 minutes of moderate exercise most days of the week.
- Maintain a Healthy Weight: Excess weight can increase pressure in the abdomen and rectum. Maintaining a healthy weight can reduce the risk of hemorrhoids.
- Proper Posture: Sit with good posture to reduce pressure on the rectum and anus.
- Avoid Prolonged Sitting: If your job requires prolonged sitting, take frequent breaks to stand up and move around.
7.5 Example Prevention Plan
| Time | Activity | Benefit |
|---|---|---|
| Morning | High-fiber breakfast (e.g., oatmeal) | Softens stool for easier bowel movements |
| Throughout Day | Drink at least 8 glasses of water | Keeps stool soft and prevents constipation |
| Lunch | Include fruits and vegetables | Adds fiber to the diet |
| Afternoon | Take a 15-minute walk | Stimulates bowel function |
| Evening | High-fiber dinner (e.g., lentil soup) | Ensures sufficient fiber intake |
| Before Bed | Drink 1 glass of water | Helps maintain hydration throughout the night |
8. Living with Hemorrhoids: Tips for Managing Daily Life
Living with hemorrhoids can be challenging, but with the right strategies, you can manage your symptoms and maintain a comfortable lifestyle.
8.1 Pain Management Techniques
- Sitz Baths: Regular sitz baths can help relieve pain and itching.
- Topical Anesthetics: Over-the-counter creams containing lidocaine can provide temporary pain relief.
- Pain Relievers: Nonsteroidal anti-inflammatory drugs (NSAIDs) like ibuprofen can help reduce pain and inflammation.
8.2 Maintaining Hygiene
- Gentle Cleaning: Clean the anal area gently with warm water and mild soap after each bowel movement.
- Avoid Irritants: Avoid using scented soaps, lotions, or wipes that can irritate the anal area.
- Pat Dry: Pat the area dry with a soft towel instead of rubbing.
8.3 Comfort Measures
- Cushioned Seats: Use a cushioned seat or donut pillow to reduce pressure on the anal area when sitting.
- Loose Clothing: Wear loose, cotton clothing to promote air circulation and reduce irritation.
- Avoid Prolonged Sitting: Take frequent breaks to stand up and move around if your job requires prolonged sitting.
8.4 Psychological Support
- Education: Understanding hemorrhoids and their management can reduce anxiety and improve coping strategies.
- Support Groups: Consider joining a support group or online forum to connect with others who have hemorrhoids.
- Counseling: If hemorrhoids are causing significant distress, consider seeking counseling or therapy.
8.5 Creating a Comfortable Environment
| Area | Strategy | Benefit |
|---|---|---|
| Bathroom | Keep soft, unscented wipes on hand | Gentle cleaning after bowel movements |
| Work | Use a cushioned seat | Reduces pressure on the anal area when sitting |
| Home | Designate a comfortable sitz bath area | Easy access for regular sitz baths |
| Wardrobe | Choose loose, cotton clothing | Promotes air circulation and reduces irritation |
9. Hemorrhoids and Pregnancy: Special Considerations
Pregnancy increases the risk of developing hemorrhoids due to hormonal changes and increased pressure on the pelvic veins. Managing hemorrhoids during pregnancy requires special consideration to ensure the health of both the mother and the baby.
9.1 Causes of Hemorrhoids During Pregnancy
- Hormonal Changes: Pregnancy hormones can relax the veins, making them more prone to swelling.
- Increased Pressure: The growing uterus puts pressure on the pelvic veins, leading to increased pressure in the rectum and anus.
- Constipation: Pregnancy can cause constipation, which increases straining during bowel movements.
- Straining During Childbirth: The act of pushing during labor can exacerbate hemorrhoids.
9.2 Safe Treatment Options During Pregnancy
- Dietary Changes: Increase fiber intake and stay hydrated to prevent constipation.
- Topical Treatments: Over-the-counter hemorrhoid creams and witch hazel wipes are generally safe to use during pregnancy.
- Sitz Baths: Regular sitz baths can help relieve pain and itching.
- Stool Softeners: If dietary changes are not enough, a doctor may recommend a stool softener to prevent constipation.
9.3 Treatments to Avoid During Pregnancy
- Certain Medications: Some hemorrhoid medications are not safe to use during pregnancy. Always consult with a doctor before taking any medication.
- Invasive Procedures: Invasive procedures like hemorrhoidectomy are generally avoided during pregnancy unless absolutely necessary.
9.4 Prevention Strategies During Pregnancy
- Prenatal Exercise: Regular exercise, such as walking or swimming, can help stimulate bowel function and prevent constipation.
- Proper Posture: Maintain good posture to reduce pressure on the pelvic veins.
- Avoid Prolonged Sitting or Standing: Take frequent breaks to move around if your job requires prolonged sitting or standing.
9.5 Creating a Pregnancy-Friendly Management Plan
| Stage | Strategy | Benefit |
|---|---|---|
| First Trimester | Focus on dietary changes and hydration | Prevents constipation and reduces pressure on veins |
| Second Trimester | Continue dietary changes and exercise | Maintains bowel regularity and supports vein health |
| Third Trimester | Use sitz baths and topical treatments | Relieves pain and itching |
| Postpartum | Continue all strategies and consult doctor | Manages hemorrhoids after childbirth and ensures proper healing |
10. When to See a Doctor: Recognizing the Need for Professional Help
While many cases of hemorrhoids can be managed with home remedies, it’s important to recognize when professional medical help is needed.
10.1 Signs That You Need to See a Doctor
- Persistent Rectal Bleeding: Any persistent bleeding should be evaluated to rule out other potential causes, such as colorectal polyps or cancer.
- Severe Pain: Intense pain that doesn’t improve with home treatment may indicate a thrombosed hemorrhoid or another condition.
- Prolapse That Cannot Be Reduced: If an internal hemorrhoid prolapses and cannot be pushed back in, seek medical attention.
- Changes in Bowel Habits: Any significant changes in bowel habits, such as persistent constipation or diarrhea, should be evaluated.
- Anemia Symptoms: If you experience symptoms of anemia, such as fatigue, weakness, or shortness of breath, due to blood loss from hemorrhoids, see a doctor.
- Uncertainty About Diagnosis: If you are unsure whether you have hemorrhoids or another condition, seek a medical evaluation.
10.2 Preparing for Your Doctor’s Appointment
- List Your Symptoms: Write down all your symptoms, including when they started and what makes them better or worse.
- List Your Medications: Bring a list of all medications, supplements, and over-the-counter products you are taking.
- List Your Medical History: Be prepared to discuss your medical history, including any previous bowel problems or surgeries.
- Write Down Questions: Prepare a list of questions to ask your doctor, such as:
- What is the cause of my hemorrhoids?
- What treatment options are available?
- What can I do to prevent future hemorrhoids?
- Are there any lifestyle changes I should make?
10.3 What to Expect During Your Appointment
- Physical Examination: The doctor will perform a physical examination, including a visual inspection of the anus and a digital rectal exam.
- Diagnostic Tests: Depending on your symptoms, the doctor may recommend additional tests, such as anoscopy or sigmoidoscopy.
- Treatment Plan: The doctor will discuss your treatment options and develop a plan tailored to your individual needs.
10.4 Follow-Up Care
- Follow Doctor’s Instructions: Follow your doctor’s instructions carefully and take all medications as prescribed.
- Schedule Follow-Up Appointments: Schedule follow-up appointments as recommended to monitor your progress and adjust your treatment plan if necessary.
- Monitor Your Symptoms: Keep track of your symptoms and report any changes to your doctor.
Navigating the world of hemorrhoids can be uncomfortable, but understanding the causes, symptoms, and available treatments can empower you to take control of your health. By adopting healthy lifestyle habits, seeking timely medical care, and managing your symptoms effectively, you can find relief and improve your quality of life.
Remember, the information provided here is for educational purposes only and is not a substitute for professional medical advice. Always consult with a qualified healthcare provider for diagnosis and treatment of any medical condition.
Do you have more questions about hemorrhoids or other health concerns? Visit why.edu.vn at 101 Curiosity Lane, Answer Town, CA 90210, United States, or contact us via Whatsapp at +1 (213) 555-0101 to find expert answers and solutions. We’re here to help you explore and understand the world around you, providing reliable and accessible information to satisfy your curiosity.
Frequently Asked Questions (FAQ) about Hemorrhoids
Here are some frequently asked questions about hemorrhoids to further enhance your understanding:
-
Are hemorrhoids contagious?
- No, hemorrhoids are not contagious. They are a result of swollen veins and are not caused by an infection that can be transmitted to others.
-
Can hemorrhoids go away on their own?
- Mild hemorrhoids can sometimes resolve on their own with lifestyle changes such as increasing fiber and water intake. However, more severe cases may require medical treatment.
-
Is it safe to use over-the-counter hemorrhoid creams during pregnancy?
- Generally, yes, but it’s always best to consult with your healthcare provider before using any medications during pregnancy to ensure they are safe for you and your baby.
-
How can I prevent constipation to avoid hemorrhoids?
- To prevent constipation, maintain a diet high in fiber, drink plenty of water, engage in regular physical activity, and avoid delaying bowel movements when you feel the urge.
-
Can sitting for long periods cause hemorrhoids?
- Yes, prolonged sitting can increase pressure on the veins in the anus and rectum, contributing to the development of hemorrhoids. Take frequent breaks to stand and move around.
-
What is a thrombosed hemorrhoid?
- A thrombosed hemorrhoid is an external hemorrhoid that has a blood clot inside it. This can cause sudden, severe pain and swelling.
-
Are there any foods I should avoid to prevent hemorrhoids?
- You may want to avoid foods that can cause constipation, such as processed foods, red meat, and dairy products. Also, limit your intake of caffeine and alcohol, which can dehydrate you.
-
Is surgery always necessary for hemorrhoids?
- No, surgery is usually reserved for severe cases that do not respond to other treatments. Many cases can be managed with lifestyle changes, home remedies, or minimally invasive procedures.
-
How long does it take for hemorrhoids to heal?
- Healing time varies depending on the severity of the hemorrhoids and the treatment method used. Mild cases may heal within a few days with home remedies, while more severe cases or surgical treatments may take several weeks.
-
Can hemorrhoids cause long-term health problems?
- Hemorrhoids themselves do not usually cause long-term health problems. However, chronic bleeding can lead to anemia, and persistent symptoms can affect your quality of life. It’s important to seek appropriate treatment to manage your symptoms.