Are my teeth translucent? This condition, often marked by a glassy or see-through appearance at the edges of your teeth, particularly near the biting surfaces, can indicate enamel erosion and potential oral health issues. At why.edu.vn, we understand the concern this can raise and aim to provide clear, actionable insights to restore your confidence. Addressing translucent teeth involves understanding the underlying causes and exploring effective treatments like dental bonding or veneers, alongside preventive measures such as fluoride treatments and dietary adjustments to protect your enamel.
1. Understanding Translucent Teeth: An Overview
Translucent teeth, characterized by a semi-clear appearance particularly along the edges, often signal a reduction in enamel thickness. This thinning can lead to increased sensitivity and a heightened risk of decay. Understanding the underlying causes is the first step toward effective management and prevention.
1.1. What Does Translucency in Teeth Indicate?
The translucent appearance of teeth is primarily an indicator of enamel thinning or erosion. Enamel, the hard, outer layer of the tooth, is responsible for protecting the underlying dentin from acids and physical wear. When enamel becomes thinner, it loses its opacity, allowing more light to pass through and giving the teeth a translucent look. This condition can be an early sign of more significant dental health issues and should not be ignored.
1.2. Common Signs and Symptoms of Translucent Teeth
Besides the visible translucency, especially at the edges of teeth, other signs and symptoms may accompany enamel erosion:
- Increased Sensitivity: Teeth may become more sensitive to hot, cold, or sweet foods and drinks.
- Rough Edges: The edges of the teeth may feel rough or uneven to the tongue.
- Yellowing: As the enamel thins, the underlying dentin, which is yellow in color, becomes more visible.
- Chipping or Cracking: Weakened enamel is more prone to chipping or cracking.
- Cavities: With less enamel protection, the teeth are more susceptible to decay and cavity formation.
1.3. Visual Examination: How to Check for Translucency
To check for translucency, examine your teeth in a well-lit area. Focus on the biting edges and tips of your teeth. If these areas appear more transparent or glassy than the rest of the tooth, it’s likely that you’re experiencing enamel thinning. Comparing your teeth to photos of healthy teeth can also help you identify any differences in appearance. Regular dental check-ups are crucial for early detection and professional evaluation.
2. Delving Deeper: Causes of Teeth Translucency
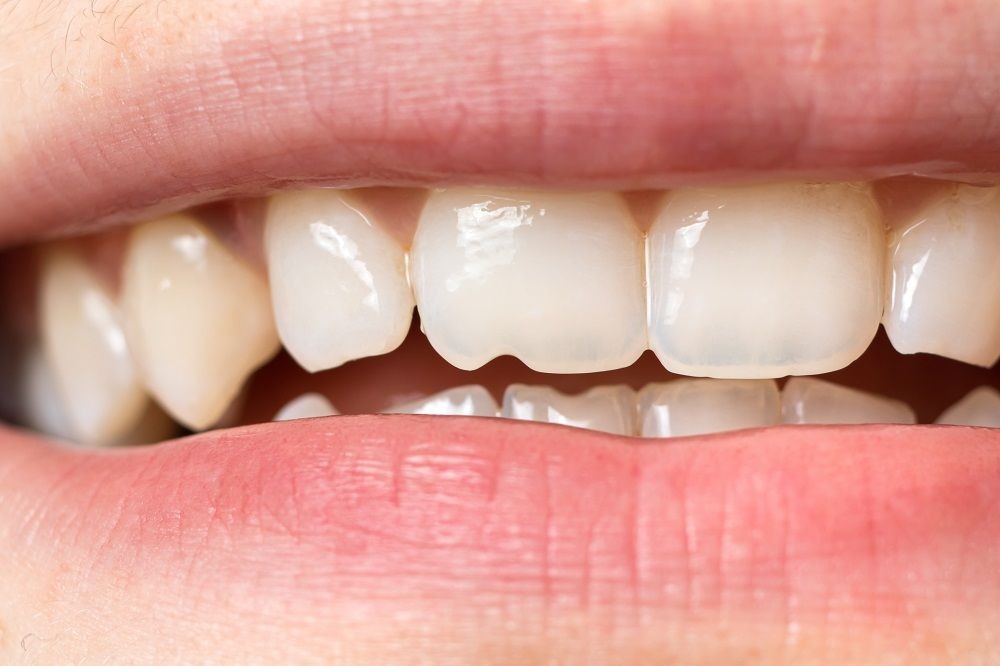 examining teeth translucency Northborough Massachusetts
examining teeth translucency Northborough Massachusetts
Several factors can contribute to the erosion of tooth enamel, leading to translucency. These range from dietary habits to genetic predispositions. Identifying the specific causes is crucial for developing an effective treatment and prevention plan.
2.1. Dietary Habits and Enamel Erosion
Diet plays a significant role in the health of your tooth enamel. Frequent consumption of acidic foods and beverages can gradually erode the enamel, leading to translucency.
2.1.1. Acidic Foods and Drinks to Watch Out For
Acidic foods and drinks can significantly impact enamel health. Items high in acidity can dissolve the minerals in tooth enamel, weakening it over time. Here are some key culprits:
- Citrus Fruits: Lemons, limes, oranges, and grapefruits are highly acidic. While they provide essential vitamins, excessive consumption can erode enamel.
- Carbonated Drinks: Sodas, energy drinks, and even sparkling water are acidic and can cause significant damage. The pH level in these drinks is often low enough to dissolve enamel.
- Fruit Juices: Many fruit juices, especially those made from citrus fruits or apples, are acidic.
- Pickled Foods: Foods pickled in vinegar, such as pickles and sauerkraut, can contribute to enamel erosion due to their high acidity.
- Wine: Both red and white wines are acidic and can erode enamel.
- Sugary Foods: Sugar itself doesn’t directly erode enamel, but it feeds bacteria in the mouth that produce acid, indirectly leading to erosion.
2.1.2. How Acid Affects Tooth Enamel
When you consume acidic foods or drinks, the acid attacks the enamel surface, a process known as demineralization. This weakens the enamel, making it more porous and susceptible to wear and tear. Over time, repeated acid attacks can lead to significant enamel loss, resulting in translucency, sensitivity, and an increased risk of cavities. The pH level in your mouth drops, creating an environment where enamel erosion is more likely to occur.
2.1.3. Balancing Diet for Optimal Enamel Health
To protect your enamel, it’s essential to balance your diet and minimize exposure to acidic substances. Here are some tips:
- Limit Acidic Foods and Drinks: Reduce your intake of citrus fruits, carbonated drinks, fruit juices, and other acidic items.
- Use a Straw: When consuming acidic beverages, use a straw to minimize contact with your teeth.
- Rinse with Water: After consuming acidic foods or drinks, rinse your mouth with water to help neutralize the acid.
- Chew Sugar-Free Gum: Chewing sugar-free gum stimulates saliva production, which helps neutralize acids and remineralize enamel.
- Eat Cheese: Cheese can help neutralize acids in the mouth and promote enamel remineralization.
- Include Calcium-Rich Foods: Incorporate calcium-rich foods like milk, yogurt, and leafy greens into your diet to strengthen enamel.
2.2. Bruxism (Teeth Grinding) and Its Impact
Bruxism, or teeth grinding, is a common condition that can significantly impact your dental health. It involves clenching or grinding your teeth, often unconsciously, which can lead to enamel erosion and other dental problems.
2.2.1. Understanding the Mechanics of Bruxism
Bruxism typically occurs during sleep but can also happen while you’re awake. The force exerted during teeth grinding can wear down the enamel, leading to a variety of dental issues. The constant friction and pressure can cause:
- Enamel Erosion: The outer layer of your teeth wears away, leading to sensitivity and translucency.
- Flattened Teeth: Teeth may become flattened or shortened due to the continuous grinding.
- Chipped or Cracked Teeth: The structural integrity of your teeth is compromised, making them more prone to damage.
- Jaw Pain: The muscles in your jaw can become sore and fatigued from the constant clenching and grinding.
- Headaches: Tension headaches are common among individuals with bruxism due to the strain on jaw muscles.
2.2.2. How Bruxism Contributes to Teeth Translucency
The primary way bruxism contributes to teeth translucency is through the physical wear of enamel. As the enamel thins, the teeth become more transparent, especially along the edges. This thinning not only affects the appearance of your teeth but also increases their sensitivity to temperature and pressure. The loss of enamel exposes the underlying dentin, which is more susceptible to decay and staining.
2.2.3. Management and Prevention Strategies for Bruxism
Managing bruxism involves addressing the underlying causes and protecting your teeth from further damage. Here are some strategies:
- Night Guards: Wearing a custom-fitted night guard is one of the most effective ways to protect your teeth from grinding during sleep. The guard acts as a barrier between your upper and lower teeth, preventing them from grinding against each other.
- Stress Management: Stress is a common trigger for bruxism. Practicing relaxation techniques such as meditation, yoga, or deep breathing exercises can help reduce teeth grinding.
- Biofeedback: This technique helps you become more aware of muscle activity and teaches you how to control it. It can be useful for reducing teeth clenching during the day.
- Medications: In some cases, muscle relaxants or anti-anxiety medications may be prescribed to reduce teeth grinding, especially if it’s related to stress or anxiety.
- Dental Adjustments: Your dentist may adjust the surface of your teeth to improve your bite and reduce the likelihood of grinding.
- Botox Injections: In severe cases, Botox injections into the jaw muscles can help relax them and reduce grinding.
2.3. Acid Reflux and Its Effects on Enamel
Acid reflux, also known as gastroesophageal reflux disease (GERD), is a condition where stomach acid flows back into the esophagus and, in some cases, into the mouth. This acid can have a detrimental effect on tooth enamel, leading to erosion and translucency.
2.3.1. The Science Behind Acid Reflux and Enamel Erosion
When stomach acid enters the mouth, it lowers the pH level, creating an acidic environment that demineralizes tooth enamel. Enamel is primarily composed of minerals, and prolonged exposure to acid can dissolve these minerals, weakening the enamel structure. The acid attack can lead to:
- Enamel Thinning: The outer layer of your teeth gradually wears away, resulting in increased sensitivity and translucency.
- Increased Risk of Cavities: Weakened enamel makes your teeth more vulnerable to decay-causing bacteria.
- Tooth Sensitivity: As enamel erodes, the underlying dentin becomes exposed, leading to sensitivity to hot, cold, and sweet stimuli.
- Changes in Tooth Shape: Teeth may develop a rounded or cupped appearance due to the acid eroding the surface.
2.3.2. Identifying Acid Reflux as a Potential Cause
If you experience frequent heartburn, regurgitation, or a sour taste in your mouth, you may have acid reflux. Other signs that acid reflux could be affecting your teeth include:
- Morning Soreness: Your teeth may feel sore or sensitive, especially in the morning.
- Dry Mouth: Acid reflux can reduce saliva production, leading to dry mouth, which exacerbates enamel erosion.
- Bad Breath: Acid reflux can cause persistent bad breath.
2.3.3. Strategies to Mitigate Acid Reflux-Related Erosion
Managing acid reflux is crucial for protecting your tooth enamel. Here are some strategies:
- Consult a Doctor: If you suspect you have acid reflux, consult a doctor for diagnosis and treatment options.
- Medications: Over-the-counter or prescription medications, such as antacids, H2 blockers, and proton pump inhibitors (PPIs), can help reduce stomach acid production.
- Dietary Changes: Avoid foods and drinks that trigger acid reflux, such as fatty foods, spicy foods, chocolate, caffeine, and alcohol.
- Smaller Meals: Eat smaller, more frequent meals instead of large meals to reduce pressure on the stomach.
- Stay Upright After Eating: Avoid lying down for at least three hours after eating to prevent acid from flowing back into the esophagus.
- Elevate Your Head: Elevate the head of your bed by 6-8 inches to help keep stomach acid from entering the esophagus during sleep.
- Dental Care: Use fluoride toothpaste and mouthwash to strengthen enamel and protect against acid erosion.
2.4. Genetic Predisposition and Enamel Formation
Genetic factors can play a significant role in the formation and quality of tooth enamel. Some individuals are genetically predisposed to having thinner or weaker enamel, making them more susceptible to translucency and erosion.
2.4.1. How Genetics Influence Enamel Quality
Genes influence various aspects of enamel development, including:
- Enamel Thickness: Some people inherit genes that result in thinner enamel, making their teeth more prone to translucency and erosion.
- Enamel Hardness: The hardness and mineral content of enamel can be genetically determined. Softer enamel is more susceptible to acid attacks and wear.
- Enamel Structure: Genes influence the organization and structure of enamel crystals. Disorganized or defective enamel is weaker and more prone to damage.
2.4.2. Genetic Conditions Affecting Enamel
Several genetic conditions can affect enamel formation, leading to enamel defects and increased translucency:
- Amelogenesis Imperfecta: This is a group of genetic disorders that affect the structure and appearance of tooth enamel. It can cause enamel to be thin, soft, discolored, or absent altogether.
- Dentinogenesis Imperfecta: This genetic condition affects the development of dentin, the layer beneath the enamel. Although it primarily affects dentin, it can also impact the enamel’s integrity and appearance.
- Ectodermal Dysplasia: This genetic disorder affects the development of ectodermal tissues, including enamel, hair, and nails. It can result in thin or poorly formed enamel.
2.4.3. Managing Genetically Predisposed Translucency
While you can’t change your genetic makeup, you can take steps to manage and protect your enamel if you’re genetically predisposed to enamel defects:
- Enhanced Oral Hygiene: Practice meticulous oral hygiene, including brushing twice a day with fluoride toothpaste, flossing daily, and using an antibacterial mouthwash.
- Fluoride Treatments: Regular fluoride treatments can help strengthen enamel and make it more resistant to acid attacks.
- Protective Dental Treatments: Consider dental treatments such as sealants, bonding, or veneers to protect and reinforce weakened enamel.
- Dietary Modifications: Limit acidic foods and drinks to minimize enamel erosion.
- Regular Dental Check-ups: Visit your dentist regularly for check-ups and professional cleanings to monitor enamel health and address any issues early.
2.5. Other Factors Contributing to Translucency
Besides diet, bruxism, acid reflux, and genetics, other factors can contribute to enamel erosion and translucency.
2.5.1. Age and Natural Enamel Wear
As you age, your tooth enamel naturally wears down over time due to normal use. This gradual erosion can lead to thinner enamel and increased translucency. The cumulative effects of chewing, grinding, and exposure to acids contribute to this wear.
2.5.2. Environmental Factors and Exposure to Chemicals
Environmental factors and exposure to certain chemicals can also impact enamel health. For example, swimming in chlorinated pools regularly can expose your teeth to acids that erode enamel. Similarly, exposure to industrial chemicals or pollutants can weaken enamel over time.
2.5.3. Over-Brushing and Improper Oral Hygiene Techniques
While good oral hygiene is essential, over-brushing or using improper techniques can actually damage your enamel. Brushing too hard or using a hard-bristled toothbrush can wear away enamel, leading to sensitivity and translucency. It’s important to use a soft-bristled toothbrush and gentle, circular motions when brushing.
3. How Translucency Affects Your Oral Health
Teeth translucency is more than just a cosmetic issue; it can have significant implications for your overall oral health. Understanding these effects can help you appreciate the importance of early intervention and proper management.
3.1. Increased Tooth Sensitivity
One of the most common and bothersome effects of teeth translucency is increased sensitivity. As enamel thins, the underlying dentin becomes exposed. Dentin contains tiny tubules that lead directly to the tooth’s nerve center, the pulp. When these tubules are exposed, they allow hot, cold, sweet, or acidic stimuli to reach the nerve more easily, causing sharp, shooting pains.
3.2. Higher Risk of Cavities and Decay
Enamel is the primary defense against tooth decay. When it thins due to erosion, your teeth become more vulnerable to bacteria and acids that cause cavities. The weakened enamel provides less protection, allowing bacteria to penetrate the tooth more easily and leading to faster decay. Areas with translucent edges are particularly susceptible to cavity formation.
3.3. Potential for Tooth Damage and Cracking
Translucent teeth are structurally weaker and more prone to damage. The thinned enamel is less able to withstand the forces of chewing and biting, making your teeth more susceptible to chipping, cracking, and fractures. This can lead to more serious dental problems that require extensive and costly treatments.
3.4. Impact on Overall Dental Health
The effects of teeth translucency can extend beyond individual teeth, impacting your overall dental health. Untreated enamel erosion can lead to a cycle of damage, where increased sensitivity and decay make it difficult to maintain proper oral hygiene. This can result in gum disease, tooth loss, and other complications that affect your ability to eat, speak, and maintain your quality of life.
4. Professional Solutions: Dental Treatments for Translucent Teeth
When dealing with translucent teeth, professional dental treatments can provide effective solutions to restore your smile and protect your oral health. These treatments range from simple procedures to more comprehensive options, depending on the extent of enamel loss and the underlying causes.
4.1. Fluoride Treatments: Strengthening Enamel
Fluoride treatments are a common and effective way to strengthen tooth enamel and prevent further erosion. Fluoride is a mineral that helps remineralize enamel, making it more resistant to acid attacks.
4.1.1. How Fluoride Works to Remineralize Enamel
Fluoride works through a process called remineralization. When enamel is exposed to acids, it loses minerals in a process called demineralization. Fluoride helps to reverse this process by depositing minerals back into the enamel, strengthening it and making it more resistant to acid. It also inhibits the growth of bacteria that cause tooth decay.
4.1.2. Types of Fluoride Treatments Available
Various fluoride treatments are available, each with its own application and effectiveness:
- Fluoride Toothpaste: Using fluoride toothpaste daily is a simple and effective way to strengthen enamel. Look for toothpaste with at least 1000 ppm (parts per million) of fluoride.
- Fluoride Mouthwash: Fluoride mouthwash can be used in addition to toothpaste to provide extra protection. It’s especially helpful for people who are prone to cavities or enamel erosion.
- Professional Fluoride Treatments: Dentists offer professional fluoride treatments in the form of gels, foams, or varnishes. These treatments contain a higher concentration of fluoride than over-the-counter products and are applied directly to the teeth.
- Fluoride Varnish: This is a concentrated fluoride treatment that is painted onto the teeth. It hardens quickly and releases fluoride over several hours.
- Fluoride Gel: Fluoride gel is applied to the teeth using a tray that is held in the mouth for a few minutes.
- Fluoride Foam: Similar to gel, fluoride foam is applied using a tray. It’s lightweight and easy to use.
4.1.3. Benefits of Regular Fluoride Application
Regular fluoride application offers several benefits:
- Strengthens Enamel: Fluoride makes enamel more resistant to acid attacks, reducing the risk of erosion and decay.
- Reverses Early Decay: Fluoride can help reverse early stages of tooth decay by remineralizing damaged enamel.
- Reduces Sensitivity: Fluoride can help reduce tooth sensitivity by blocking the tubules in dentin.
- Prevents Cavities: By strengthening enamel and inhibiting bacteria, fluoride helps prevent cavity formation.
4.2. Dental Bonding: Restoring Tooth Structure
Dental bonding is a cosmetic dental procedure that involves applying a tooth-colored resin material to the teeth to restore their structure and improve their appearance. It’s a versatile and relatively simple treatment option for addressing translucent teeth.
4.2.1. The Bonding Process Explained
The dental bonding process typically involves the following steps:
- Preparation: The dentist will first prepare the tooth surface by slightly etching it with a mild acid. This creates a rough surface that allows the bonding material to adhere better.
- Application of Bonding Agent: A bonding agent is applied to the etched surface. This agent helps the resin material bond to the tooth.
- Resin Application: The tooth-colored resin material is applied to the tooth in layers. The dentist carefully shapes and molds the resin to achieve the desired shape and appearance.
- Curing: A special light is used to harden or cure the resin material. This process takes just a few minutes.
- Polishing: Once the resin is hardened, the dentist will polish it to create a smooth, natural-looking surface.
4.2.2. How Bonding Addresses Translucency
Dental bonding can effectively address translucency by adding a layer of opaque resin material to the teeth. This covers the translucent areas and restores the tooth’s natural appearance. Bonding can also be used to repair chipped or cracked teeth, close gaps between teeth, and improve the overall shape and size of teeth.
4.2.3. Advantages and Limitations of Bonding
Advantages:
- Cost-Effective: Dental bonding is generally less expensive than other cosmetic dental treatments like veneers or crowns.
- Non-Invasive: The procedure is minimally invasive and usually doesn’t require anesthesia.
- Quick: Bonding can typically be completed in one dental visit.
- Natural-Looking: The tooth-colored resin material can be matched to the natural shade of your teeth for a seamless appearance.
Limitations:
- Durability: Bonding is not as durable as other options like veneers or crowns. It can chip or stain over time and may need to be replaced every few years.
- Staining: The resin material is susceptible to staining from foods and drinks like coffee, tea, and red wine.
- Strength: Bonding is not as strong as natural enamel and may not be suitable for repairing large areas of damage.
4.3. Veneers: A More Permanent Solution
Veneers are thin, custom-made shells that are bonded to the front surface of your teeth to improve their appearance. They are a more permanent and durable solution for addressing translucent teeth compared to bonding.
4.3.1. Types of Veneers: Porcelain vs. Composite
There are two main types of veneers:
- Porcelain Veneers: These are made from a high-quality ceramic material that closely resembles natural tooth enamel. Porcelain veneers are highly durable, stain-resistant, and natural-looking.
- Composite Veneers: These are made from the same resin material used in dental bonding. Composite veneers are less expensive than porcelain veneers but are also less durable and more prone to staining.
4.3.2. The Veneer Application Process
The veneer application process typically involves the following steps:
- Consultation: The dentist will evaluate your teeth and discuss your goals to determine if veneers are the right treatment option for you.
- Preparation: A small amount of enamel is removed from the front surface of your teeth to make room for the veneers. This step is usually necessary for porcelain veneers but may not be required for some types of composite veneers.
- Impressions: Impressions of your teeth are taken and sent to a dental lab where the veneers are custom-made.
- Temporary Veneers: Temporary veneers may be placed on your teeth while you wait for the permanent veneers to be তৈরি.
- Bonding: Once the permanent veneers are ready, they are bonded to your teeth using a special adhesive.
- Adjustments: The dentist will make any necessary adjustments to ensure the veneers fit properly and look natural.
4.3.3. Benefits and Considerations of Veneers
Benefits:
- Durability: Porcelain veneers are highly durable and can last for many years with proper care.
- Stain Resistance: Porcelain veneers are stain-resistant, so they maintain their natural appearance over time.
- Natural-Looking: Veneers closely resemble natural tooth enamel and can significantly improve the appearance of your smile.
- Versatile: Veneers can be used to address a variety of cosmetic issues, including translucency, chipped teeth, gaps between teeth, and discoloration.
Considerations:
- Cost: Veneers are more expensive than dental bonding.
- Irreversible: The removal of enamel is usually required for porcelain veneers, making the procedure irreversible.
- Sensitivity: Some people may experience increased tooth sensitivity after getting veneers.
- Maintenance: Veneers require good oral hygiene and regular dental check-ups to maintain their appearance and longevity.
4.4. Crowns: Restoring Severely Damaged Teeth
Crowns, also known as caps, are dental restorations that cover the entire visible portion of a tooth. They are used to restore severely damaged, decayed, or weakened teeth and can be an option for addressing translucent teeth when the enamel loss is extensive.
4.4.1. When Crowns Are Necessary
Crowns may be necessary in the following situations:
- Extensive Enamel Erosion: When enamel loss is severe and has compromised the structure of the tooth.
- Severe Decay: When a tooth has extensive decay that cannot be repaired with a filling.
- Cracked or Fractured Teeth: When a tooth is cracked or fractured and needs to be reinforced.
- Root Canal Treatment: After a root canal, a crown is often placed to protect and strengthen the tooth.
4.4.2. The Crown Placement Procedure
The crown placement procedure typically involves the following steps:
- Examination and Preparation: The dentist will examine the tooth and take X-rays to assess its condition. The tooth will be prepared by removing any decay and shaping it to accommodate the crown.
- Impressions: Impressions of your teeth are taken and sent to a dental lab where the crown is custom-made.
- Temporary Crown: A temporary crown is placed on the prepared tooth while you wait for the permanent crown to be তৈরি.
- Permanent Crown Placement: Once the permanent crown is ready, it is placed on the prepared tooth and cemented into place.
- Adjustments: The dentist will make any necessary adjustments to ensure the crown fits properly and feels comfortable.
4.4.3. Types of Crowns and Their Benefits
Various types of crowns are available, each with its own benefits:
- Porcelain Crowns: These are made entirely of porcelain and offer a natural-looking appearance. They are a good choice for front teeth.
- Porcelain-Fused-to-Metal Crowns: These crowns have a metal base covered with porcelain. They are strong and durable and can be used for both front and back teeth.
- Metal Crowns: These are made entirely of metal, such as gold or silver. They are very strong and durable but do not look as natural as porcelain crowns.
- Zirconia Crowns: These are made from a strong, biocompatible ceramic material. They offer a good balance of strength and aesthetics.
Benefits of Crowns:
- Restores Tooth Structure: Crowns restore the structure and function of damaged teeth.
- Protects Weakened Teeth: Crowns protect weakened teeth from further damage.
- Improves Appearance: Crowns can improve the appearance of teeth by covering discoloration, chips, and cracks.
- Long-Lasting: Crowns can last for many years with proper care.
5. Preventive Strategies: Maintaining Healthy Enamel
While professional treatments can restore and protect translucent teeth, prevention is key to maintaining healthy enamel and preventing future problems. By adopting good oral hygiene habits and making lifestyle changes, you can significantly reduce the risk of enamel erosion and translucency.
5.1. Optimal Oral Hygiene Practices
Good oral hygiene is the foundation of healthy enamel. Regular and proper brushing, flossing, and rinsing can help remove plaque and bacteria that contribute to enamel erosion.
5.1.1. Brushing Techniques and Recommendations
Proper brushing is essential for removing plaque and bacteria from your teeth. Here are some recommendations:
- Use a Soft-Bristled Toothbrush: A soft-bristled toothbrush is gentle on enamel and gums.
- Use Fluoride Toothpaste: Fluoride toothpaste helps strengthen enamel and prevent decay.
- Brush Twice a Day: Brush your teeth for at least two minutes in the morning and before bed.
- Use Gentle, Circular Motions: Avoid brushing too hard or scrubbing, as this can damage enamel and gums. Use gentle, circular motions to clean all surfaces of your teeth.
- Clean All Surfaces: Make sure to clean the front, back, and top surfaces of each tooth.
- Replace Your Toothbrush Regularly: Replace your toothbrush every three to four months, or sooner if the bristles are frayed.
5.1.2. The Importance of Flossing Daily
Flossing is crucial for removing plaque and food particles from between your teeth, where a toothbrush can’t reach. Here are some tips for effective flossing:
- Floss Once a Day: Floss at least once a day, preferably before bed.
- Use the Right Technique: Use a gentle sawing motion to guide the floss between your teeth. Curve the floss around each tooth and slide it gently under the gumline.
- Use Enough Floss: Use about 18 inches of floss each time.
- Be Gentle: Avoid snapping the floss against your gums, as this can cause irritation and bleeding.
5.1.3. Rinsing with Fluoride Mouthwash
Rinsing with fluoride mouthwash can provide extra protection against enamel erosion and decay. Look for a mouthwash that contains fluoride and is alcohol-free. Rinse your mouth with mouthwash after brushing and flossing.
5.2. Dietary Adjustments for Enamel Protection
Your diet plays a significant role in the health of your enamel. Making dietary adjustments can help protect your enamel from acid attacks and promote remineralization.
5.2.1. Limiting Acidic Food and Beverage Consumption
Reducing your intake of acidic foods and beverages is crucial for protecting your enamel. Limit your consumption of citrus fruits, carbonated drinks, fruit juices, and other acidic items.
5.2.2. Choosing Enamel-Friendly Foods
Certain foods can help protect and strengthen your enamel. These include:
- Dairy Products: Milk, cheese, and yogurt are rich in calcium and help neutralize acids in the mouth.
- Crunchy Fruits and Vegetables: Apples, carrots, and celery stimulate saliva production and help clean your teeth.
- Leafy Greens: Spinach, kale, and other leafy greens are rich in vitamins and minerals that support oral health.
- Nuts and Seeds: Almonds, walnuts, and sesame seeds are good sources of calcium and other minerals.
5.2.3. Hydration and Saliva Production
Staying hydrated is essential for saliva production. Saliva helps neutralize acids, remineralize enamel, and wash away food particles and bacteria. Drink plenty of water throughout the day to keep your mouth hydrated.
5.3. Regular Dental Check-Ups and Professional Cleanings
Regular dental check-ups and professional cleanings are crucial for maintaining healthy enamel and detecting problems early. Your dentist can assess the condition of your enamel, identify any signs of erosion, and recommend appropriate treatments. Professional cleanings remove plaque and tartar that can contribute to enamel erosion.
5.4. Addressing Underlying Medical Conditions
Certain medical conditions, such as acid reflux and eating disorders, can contribute to enamel erosion. Addressing these underlying conditions is essential for protecting your enamel.
5.4.1. Managing Acid Reflux
If you have acid reflux, work with your doctor to manage the condition and reduce the amount of acid that enters your mouth. This may involve lifestyle changes, medications, or other treatments.
5.4.2. Seeking Help for Eating Disorders
Eating disorders like bulimia can cause severe enamel erosion due to frequent vomiting. Seeking professional help for eating disorders is essential for protecting your oral health and overall well-being.
6. Addressing Common Concerns and Misconceptions
When it comes to translucent teeth, several concerns and misconceptions can arise. Addressing these can help you make informed decisions about your oral health and treatment options.
6.1. Can Enamel Grow Back?
One of the most common questions about enamel erosion is whether enamel can grow back. Unfortunately, enamel does not have the ability to regenerate or repair itself. Once enamel is lost, it’s gone for good. This is why prevention is so important. While enamel cannot grow back, fluoride can help remineralize and strengthen the remaining enamel, making it more resistant to acid attacks.
6.2. Is Translucency Always a Sign of a Serious Problem?
While translucency is often a sign of enamel erosion, it’s not always indicative of a serious problem. In some cases, slight translucency may be due to natural variations in enamel thickness or tooth structure. However, it’s always best to consult with your dentist to determine the cause of translucency and whether any treatment is necessary.
6.3. Over-the-Counter Products vs. Professional Treatments
Many over-the-counter products claim to strengthen enamel and protect against erosion. While these products can be helpful, they are not a substitute for professional treatments. Over-the-counter fluoride toothpaste and mouthwash can help strengthen enamel, but they may not be enough to address severe enamel loss. Professional fluoride treatments, bonding, veneers, and crowns can provide more comprehensive solutions for restoring and protecting translucent teeth.
6.4. The Role of Whitening in Translucent Teeth
Teeth whitening can be a popular option for improving the appearance of discolored teeth. However, it’s important to consider the role of whitening in translucent teeth. Whitening treatments can sometimes make translucency more noticeable by further thinning the enamel. If you have translucent teeth, it’s best to consult with your dentist before undergoing any whitening treatments. They can recommend the safest and most effective options for improving the appearance of your smile.
7. The Importance of Early Detection and Intervention
Early detection and intervention are crucial for managing translucent teeth and preventing further damage. By recognizing the signs of enamel erosion and seeking timely treatment, you can protect your oral health and maintain a healthy, beautiful smile.
7.1. Recognizing Early Signs of Enamel Erosion
Being able to recognize the early signs of enamel erosion is the first step toward preventing further damage. Look out for the following signs:
- Increased Sensitivity: Teeth become more sensitive to hot, cold, or sweet foods and drinks.
- Rough Edges: The edges of the teeth feel rough or uneven.
- Yellowing: The teeth appear more yellow as the enamel thins and the underlying dentin becomes more visible.
- Translucency: The edges of the teeth appear more transparent or glassy.
7.2. Seeking Timely Dental Care
If you notice any of these signs, it’s important to seek timely dental care. Your dentist can evaluate the condition of your enamel, identify the underlying causes of erosion, and recommend appropriate treatments. Early intervention can help prevent further enamel loss and protect your teeth from decay and damage.
7.3. Long-Term Benefits of Early Intervention
Early intervention offers several long-term benefits:
- Preserves Enamel: Early treatment can help preserve the remaining enamel and prevent further erosion.
- Reduces Sensitivity: By strengthening enamel and protecting dentin, early intervention can reduce tooth sensitivity.
- Prevents Decay: Early treatment can help prevent cavities and decay by strengthening enamel and inhibiting bacteria.
- Maintains Aesthetics: Early intervention can help maintain the natural appearance of your smile.
- Saves Money: Addressing enamel erosion early can prevent the need for more extensive and costly treatments in the future.
8. Finding the Right Dental Professional
Choosing the right dental professional is essential for managing translucent teeth and protecting your oral health. A qualified and experienced dentist can provide accurate diagnoses, effective treatments, and personalized recommendations for maintaining healthy enamel.
8.1. Qualifications and Experience to Look For
When choosing a dentist, look for the following qualifications and experience:
- Education and Training: Make sure the dentist has a degree from an accredited dental school and has completed any necessary postgraduate training.
- Experience with Cosmetic Dentistry: If you’re considering cosmetic treatments like bonding or veneers, choose a dentist with experience in cosmetic dentistry.
- Experience with Enamel Erosion: Look for a dentist who has experience diagnosing and treating enamel erosion.
- Continuing Education: Choose a dentist who stays up-to-date with the latest advances in dental care through continuing education courses.
8.2. The Importance of a Comprehensive Examination
A comprehensive dental examination is crucial for accurately diagnosing the cause of translucent teeth and developing an effective treatment plan. The examination should include:
- Visual Examination: The dentist will visually examine your teeth for signs of enamel erosion, decay, and damage.
- X-Rays: X-rays can help the dentist assess the condition of your teeth and identify any underlying problems.
- Medical History: The dentist will ask about your medical history, including any medical conditions or medications that may contribute to enamel erosion.
- Dietary Assessment: The dentist may ask about your dietary habits to identify any acidic foods or drinks that may be contributing to enamel erosion.
- Bite Evaluation: The dentist will evaluate your bite to determine if bruxism or other bite problems are contributing to enamel erosion.
8.3. Building a Long-Term Relationship with Your Dentist
Building a long-term relationship with your dentist
